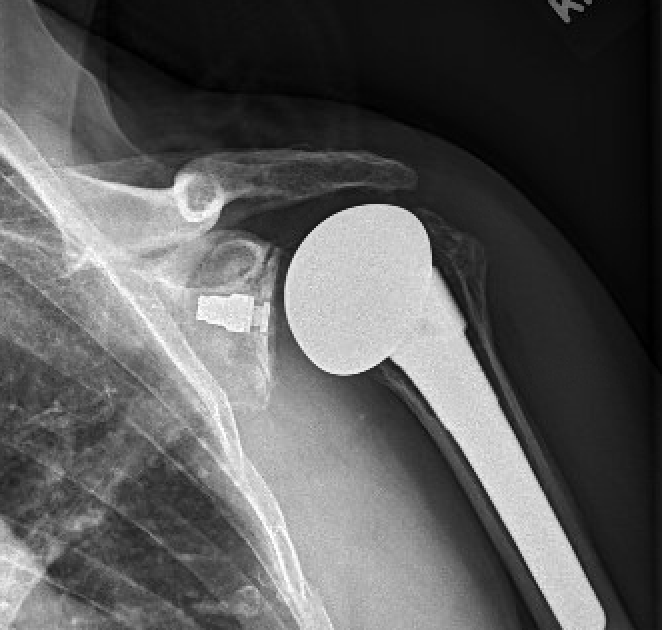
These data point to the steadily increasing number of patients having revision for arthroplasty failure, the economic burden of these revisions, and the need for an increasing number of surgeons who are equipped to manage these failures. Of importance is that these data reflect the incidence of revision per 100,000 people (not the rate of revisions for patients having shoulder arthroplasty). In that the number of shoulder arthroplasties performed per 100,000 people is steadily increasing each year, it is intuitive that the number of revisions per 100,000 people would also increase each year.
It seems that the questions of greatest importance are not addressed in this study:
1. Are patients undergoing TSA today at greater risk for complications than patients a decade ago? If so, is this a consequence of applying shoulder arthroplasty to younger patients, patients with more complex diagnoses, and patients with poorer overall health? Or is this a consequence of less experienced surgeons performing an increasing number of these procedures?
2. What are the specific failure modes driving revisions, and are those modes changing over time? For anatomic TSA, are the rates of glenoid component loosening, instability, rotator cuff failure, and infection getting higher, lower or staying the same? For reverse TSA how are the rates of instability and dislocation, acromial and scapular spine fracture, infection, notching with component loosening, and periprosthetic fracture changing with time?
3. Which patient and surgical factors are associated with each distinct failure mode? Risk factors differ by failure mode; we need to understand these associations as we strive to reduce the risk of each type of failure. Aggregating across all causes of revision in a single regression model — as most administrative database studies must do — destroys the signal. The predictors of infection-related revision are nutritional status, glycemic control, obesity, prior surgery, and prophylaxis adequacy. The predictors of instability-related revision in rTSA involve the surgeon’s choices of component design, version and inclination and approaches to soft tissue tensioning. The predictors of acromial fracture involve bone mineral density, scapular morphology, type of arthritis, prior surgery, rotator cuff status, component lateralization, and deltoid tensioning.
In that the surgeon is the method, surgeon knowledge, training, and experience deserve special study across all failure modes. These may be the most important modifiable risk factors — yet they receives minimal attention in a literature preoccupied with implant selection and surgical technology.
4. What might be done differently to prevent each type of failure? This is the most important question and the hardest to study, because it requires honest counterfactual analysis rather than statistical association. It asks not merely which factors correlate with failure, but which specific decisions — patient selection, perioperative optimization, surgical technique, rehabilitation protocol — were modifiable and, if modified, would plausibly have prevented the need for revision.
Answering this question at scale will be difficult, requiring mandatory registries with standardized failure mode coding and linkage between primary and revision procedures.
Recognizing that failure modes differ by surgeon and practice, an immediately applicable and practical approach is analogous to aviation crash analysis. Each surgeon analyzes their failures by comparing each revision to matched non-revised controls from their practice. (See How a surgeon can learn from their own adverse outcomes – an example of intrapractice analysis in reverse shoulder arthroplasty.)
A final question: is the most cost-effective approach to reducing the risk of arthroplasty complications and revisions (A) more expensive technology or (B) better surgeon training (see How much precision do we need to pay for in shoulder arthroplasty?)
A risk factor for small bird adverse outcomes in my backyard.

Cooper’s Hawk
2021
Follow on twitter/X: https://x.com/RickMatsen
Follow on facebook: https://www.facebook.com/shoulder.arthritis
Follow on LinkedIn: https://www.linkedin.com/in/rick-matsen-88b1a8133/
Here are some videos that are of shoulder interest
Shoulder arthritis – what you need to know (see this link).
How to x-ray the shoulder (see this link).
The ream and run procedure (see this link).
The total shoulder arthroplasty (see this link).
The cuff tear arthropathy arthroplasty (see this link).
The reverse total shoulder arthroplasty (see this link).
The smooth and move procedure for irreparable rotator cuff tears (see this link)
Shoulder rehabilitation exercises (see this link).